
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/viewarticle/z-drugs-disordered-sleep-early-pregnancy-new-safety-data-2025a10010sp
via IFTTT

from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/viewarticle/z-drugs-disordered-sleep-early-pregnancy-new-safety-data-2025a10010sp
via IFTTT

from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/viewarticle/early-breastfeeding-protects-preschool-mental-health-2025a10010iy
via IFTTT
Today, death rates after weight-loss surgery are considered to be “very low,” occurring in perhaps 1 in 300 to 1 in 500 patients on average.
The treatment of obesity has long been stained by the snake-oil swindling of profiteers, hustlers, and quacks. Even the modern field of bariatric medicine (derived from the Greek word baros, meaning “weight”) is pervaded by an “insidious image of sleaze.” Beguiled by advertising for fairy tale magic bullets of rapid, effortless weight loss, people blame themselves for failing to manifest the miracle or imagine themselves metabolically broken. On the other end of the spectrum are overly pessimistic practitioners of the opinion that “people who are fat are born fat, and nothing much can be done about it.” The truth lies somewhere in between.
The difficulty of curing obesity has been compared to learning a foreign language. It’s an achievement virtually anyone can attain with a sufficient investment of energies, “but it always takes a considerable amount of time and trouble.” And, of those who do stick with it, most will regain much of the weight lost. To me, this speaks to the difficulty, rather than the futility. It may take smokers an average of 30 attempts to finally kick the habit. Like quitting smoking, curing obesity is just something that has to be done. As the chair of the Association for the Study of Obesity put it, it doesn’t take “will power” to do essential tasks like getting up at night to feed a baby; it’s just something that has to be done.
Our collective response doesn’t seem to match the rhetoric or reality. If obesity is such a “national crisis” reaching alarming proportions, dubbed by the post-9/11 Surgeon General as “every bit as devastating as terrorism,” why has our reaction been so tepid? For example, governments meekly suggest the food industry take “voluntary initiatives to restrict the marketing of less healthy food options to children….” Have we just given up and ceded control?
Our timid response to the obesity epidemic is encapsulated by a national initiative promulgated by a Joint Task Force of the American Society for Nutrition, Institute of Food Technologists, and International Food Information Council: the “small-changes approach.” Since “small changes are more feasible to achieve,” suggestions include “using mustard instead of mayonnaise” and “eating 1 rather than 2 doughnuts in the morning.” Seems a bit like bringing a butter knife to a gunfight. Proponents of the small-changes approach lament that, unlike other addictions—for example, alcohol, cocaine, gambling, or tobacco—we can’t counsel our obese patients to give up the addictive element completely, as “[n]o one can give up eating.” But just because we have to breathe, doesn’t mean it has to be through the end of a cigarette. And just because we have to eat doesn’t mean we have to eat junk.
What about bringing a scalpel to the gunfight instead? The use of bariatric surgery has exploded from about 40,000 procedures noted in the first international survey in 1998 to hundreds of thousands performed now every year in the United States alone. The first technique that was developed, the intestinal bypass, involved carving out about 19 feet of intestines. More than 30,000 intestinal bypass operations were performed before we recognized “catastrophic” and “disastrous outcomes” resulted from these procedures. This included protein deficiency-induced liver disease, “which often progressed to liver failure and death.” This inauspicious start is remembered as “one of the dark blots in the history of surgery,” as I discuss in my video The Mortality Rate of Bariatric Weight-Loss Surgery.
Today, death rates after bariatric surgery are considered “very low,” occurring on average in perhaps 1 in 300 to impacting 1 in 500 patients. The most common procedure is stomach stapling, also known as sleeve gastrectomy, in which most of the stomach is permanently removed. Only a narrow tube of the stomach is left so as to restrict how much food people can eat at any one time. It’s ironic that many patients choose bariatric surgery convinced that, “for them, ‘diets do not work,’” when, in reality, that’s all the surgery may be—an enforced diet. Bariatric surgery can be thought of as a form of internal jaw wiring.
Gastric bypass, known as Roux-en-Y gastric bypass, is the second most common bariatric surgery. It combines restriction—stapling the stomach into a pouch smaller than a golf ball—with malabsorption by rearranging one’s anatomy to bypass the first part of the small intestine. It appears to be more effective than just cutting out most of the stomach, resulting in a loss of about 63% of excess weight compared to 53% with a gastric sleeve. But gastric bypass carries a greater risk of serious complications. Many are surprised to learn that new “surgical procedures…do not require premarket testing and approval by the Food and Drug Administration (FDA)” and are largely exempt from rigorous regulatory scrutiny.
Doctor’s Note
I didn’t know there wasn’t some kind of approval process for new surgical procedures!
This is the first video in a four-part series on bariatric surgery. Coming up are:
My book How Not to Diet is focused exclusively on sustainable weight loss. Check it out from your local public library or pick it up from wherever you get your books. (All proceeds from my books are donated to charity.)
from NutritionFacts.org https://nutritionfacts.org/blog/bariatric-weight-loss-surgery-and-mortality/
via IFTTT
How do barukas, also known as baru almonds, compare with other nuts?
There is a new nut on the market called baru almonds, branded as “barukas” or baru nuts. Technically, it isn’t a nut but a seed native to the Brazilian Savannah, known as the Cerrado, which is now among the most threatened ecosystems on the planet. Over the last 30 years, much of the Cerrado’s ecosystem has been destroyed by extensive cattle ranching and feed crop production to fatten said cattle. If it were profitable not to cut down the native trees and instead sell baru nuts, for example, that could be good for the ecosystem’s health. But what about our health?
“Although baru nuts are popular and widely consumed, few studies report on their biological properties.” They do have a lot of polyphenol phytonutrients, presumably accounting for their high antioxidant activity. (About 90% of their phytonutrients are present in the peel.) Are they nutritious? Yes, but do they have any special health benefits—beyond treating chubby mice?
Researchers found that individuals fed baru nuts showed lower cholesterol, supposedly indicating the nuts “have great potential for dietary use” in preventing and controlling cholesterol problems. But the individuals were rats, not humans, and the baru nuts were compared to lard. Pretty much everything lowers cholesterol compared to lard. Nevertheless, there haven’t been any reports about the effect of baru nut consumption on human health, until this: A randomized, controlled study of humans found that eating less than an ounce a day for six weeks led to a 9% drop in LDL cholesterol. Twenty grams would be about 15 nuts or a palmful.
Like many other nut studies, even though the research subjects were told to add nuts to their regular diets, there was no weight gain, presumably because nuts are so filling that we inadvertently cut down on other foods throughout the day. How good is a 9.4% drop in LDL? It’s the kind of drop we can get from regular almonds, though macadamias and pistachios may work even better, but those were at much higher doses. It appears that 20 grams of baru nuts work as well as 73 grams of almonds. So, on a per-serving basis or a per-calorie basis, baru nuts really did seem to be special.
There are lower-dose nut studies that show similar or even better results. In this one, for instance, people were given 25 grams of almonds for just four weeks and got about a 6% drop in their LDL cholesterol. In another study, after consuming just 10 grams of almonds a day, or just seven individual almonds a day, study participants got more like a 30% drop in LDL during the same time frame as the baru nuts. Three times better LDL at half the dose with regular almonds, as you can see below and at 2:47 in my video Are Baruka Nuts the Healthiest Nut?.
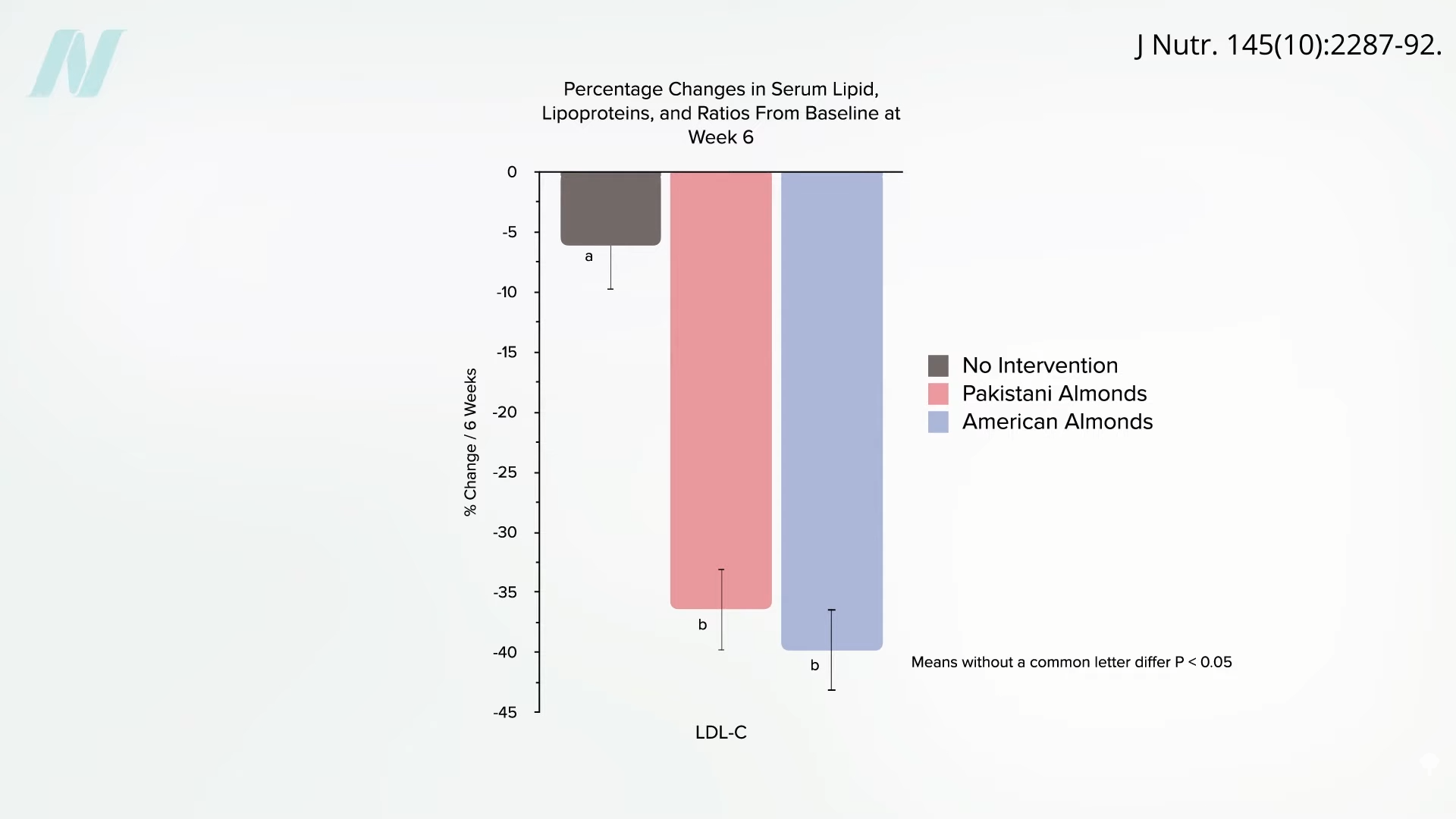
The biggest reason we are more confident in regular almonds than baru almonds is that studies have been done over and over in more than a dozen randomized controlled trials, whereas in the only other cholesterol trial of baru nuts, researchers found no significant benefit for LDL cholesterol, even at the same 20-gram dose given for even longer—a period of eight weeks.
That’s disappointing, but it isn’t the primary reason I would suggest choosing other nuts instead of baru nuts. I would do so because we can’t get raw baru nuts. They contain certain compounds that must be inactivated by heat before we can eat them. The reason raw nuts are preferable is because of advanced glycation end-products (AGEs), so-called glycotoxins, which are known to contribute to increased oxidative stress and inflammation.
Glycotoxins are naturally present in uncooked animal-derived foods, and dry-heat cooking like grilling can make things worse. The three highest recorded levels have been in bacon, broiled hot dogs, and roasted barbecued chicken skin—nothing even comes close to that, not even Chicken McNuggets, as you can see below and at 3:50 in my video.
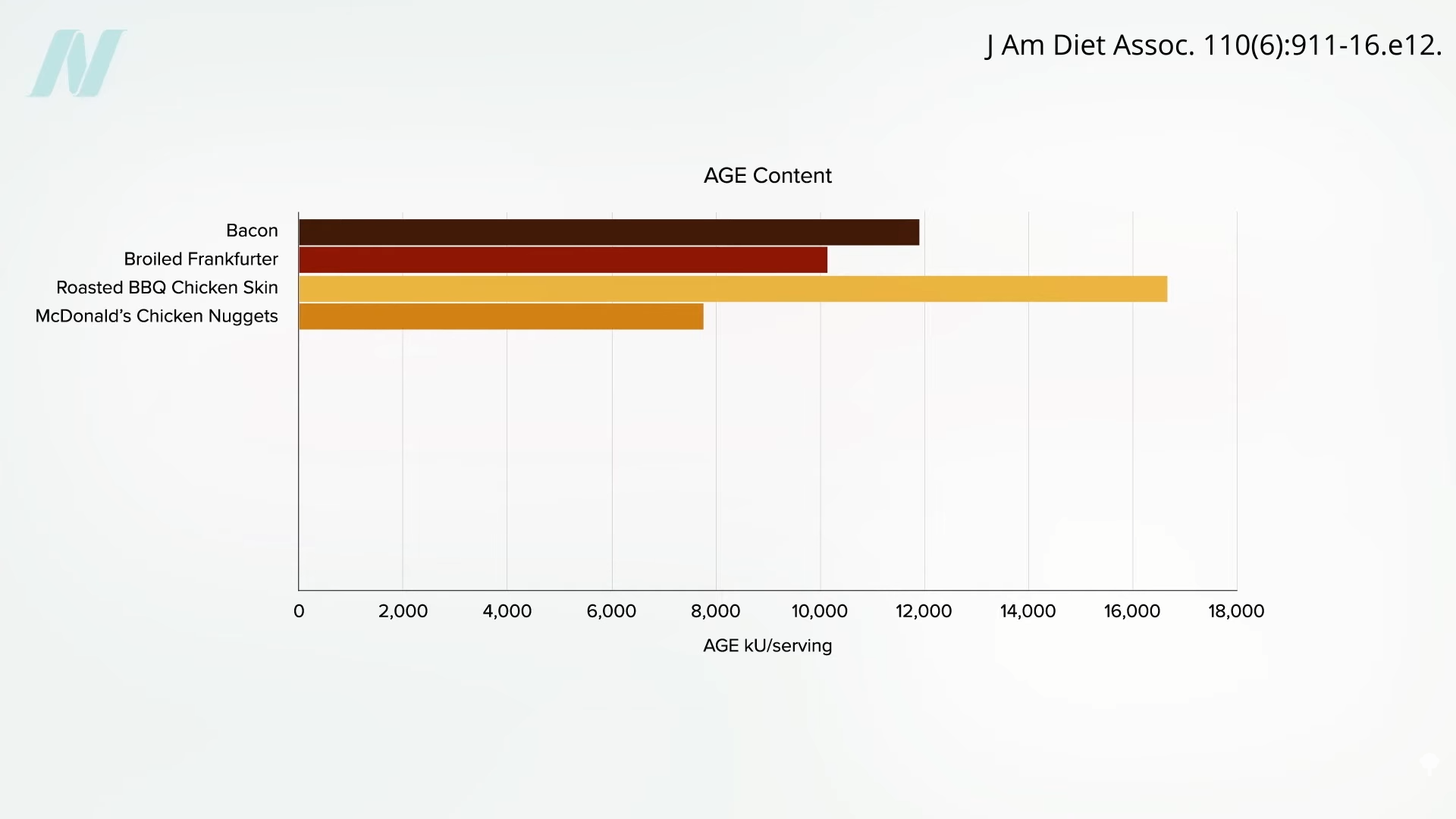
However, any foods high in fat and protein can create AGEs at high enough temperatures. So, although plant foods tend to “contain relatively few AGEs, even after cooking,” there are some high-fat, high-protein plant foods. But, again, AGEs aren’t a problem at all with most plant foods. See the AGE content in boiled tofu (in a soup, for instance), broiled tofu, a raw apple, a baked apple, a veggie burger—I was surprised that veggie burgers are so low in AGEs, even when baked or fried—and nuts and seeds, which are up in tofu territory, especially when roasted, which is why I would recommend raw nuts and seeds and nut and seed butters whenever you have a choice. See below and at 4:33 in my video.
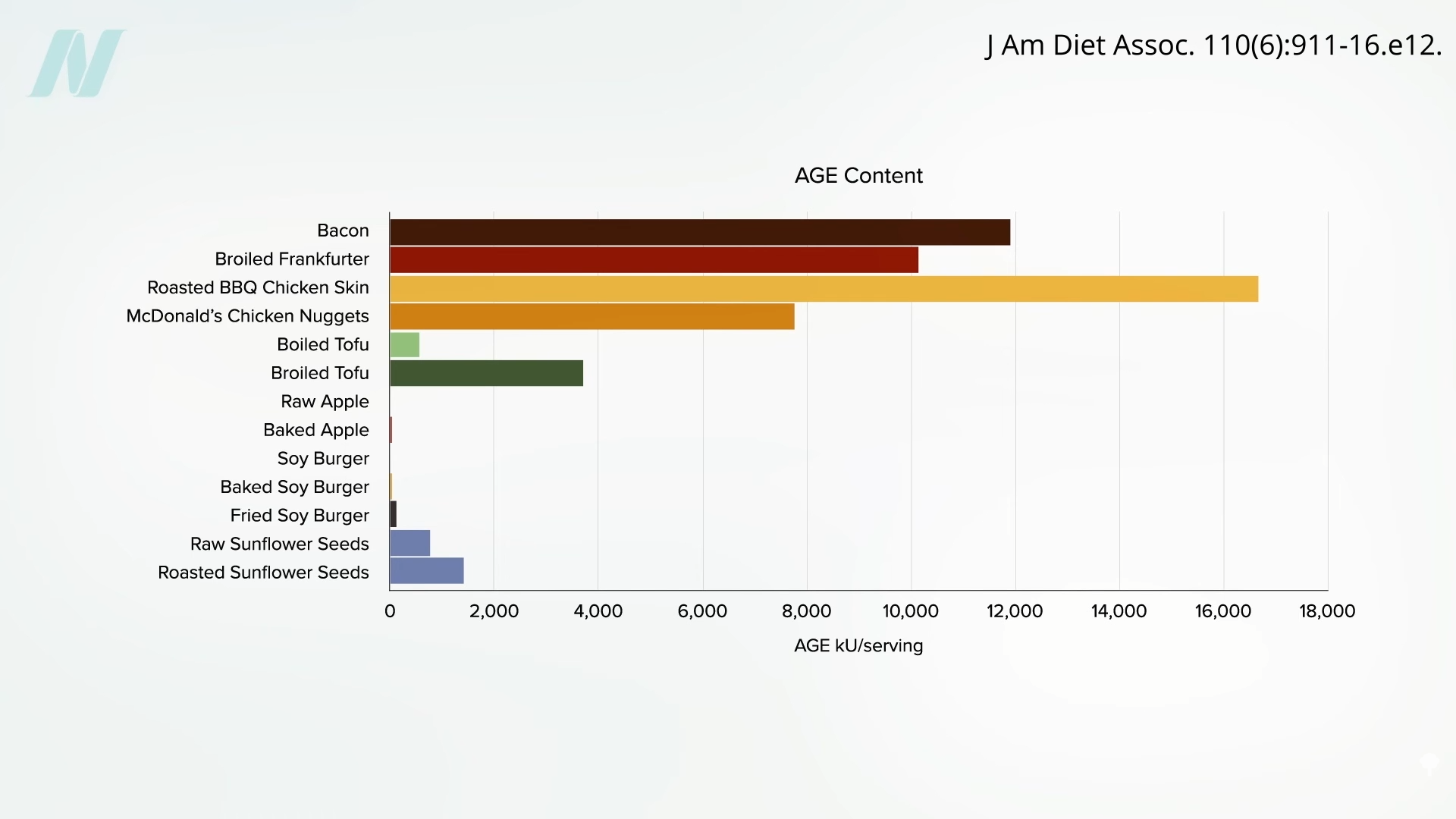
Doctor’s Note
In my Daily Dozen checklist, I recommend eating a quarter cup of nuts or seeds or two tablespoons of nut or seed butter each day. Why? See related posts below.
For those unfamiliar with advanced glycation end-products (AGEs), check out the first two videos I did on them way back when: Glycotoxins and Avoiding Glycotoxins in Food.
from NutritionFacts.org https://nutritionfacts.org/blog/how-healthy-are-baruka-nuts/
via IFTTT
If the microbiome of those eating plant-based diets protects against the toxic effects of TMAO, what about swapping gut flora?
“Almost 2,500 years ago, Hippocrates stated that ‘All disease begins in the gut.’” When we feed our gut bacteria right with whole plant foods, they feed us right back with beneficial compounds like butyrate, which our gut bugs make from fiber. On the other hand, if we feed them wrong, they can produce detrimental compounds like TMAO, which they make from cheese, eggs, seafood, and other meat.
We used to think that TMAO only contributed to cardiovascular diseases, like heart disease and stroke, but, more recently, it has been linked to psoriatic arthritis, associated with polycystic ovary syndrome, and everything in between. I’m most concerned about our leading killers, though. Of the top ten causes of death in the United States, we’ve known about its association with increased risk of heart disease and stroke, killers number one and five, but recently, an association has also been found between blood levels of TMAO and the risks of various cancers, which are our killer number two. The link between TMAO and cancer could be attributed to the inflammation caused by TMAO, but it could also be oxidative stress (free radicals), DNA damage, or a disruption in protein folding.
What about our fourth leading killer, chronic obstructive pulmonary disease (COPD), like emphysema? TMAO is associated with premature death in patients with exacerbated COPD, though it’s suspected that it’s due to them dying from more cardiovascular disease.
The link to stroke is a no-brainer—no pun intended. It is due to the higher blood pressure associated with higher TMAO levels, as well as the greater likelihood of clots forming in those with atrial fibrillation. Those with higher TMAO levels also appear to have worse strokes and four times the odds of death.
Killer number six is Alzheimer’s disease. Can TMAO even get up into our brains? Yes, TMAO is present in human cerebrospinal fluid, which bathes the brain, and TMAO levels are higher in those with mild cognitive dysfunction and those with Alzheimer’s disease dementia. “In the brain, TMAO has been shown to induce neuronal senescence [meaning, deterioration with age], increase oxidative stress, impair mitochondrial function, and inhibit mTOR signaling, all of which contribute to brain aging and cognitive impairment.”
Killer number seven is diabetes, and people with higher TMAO levels are about 50% more likely to have diabetes. Killer number eight is pneumonia, and TMAO predicts fatal outcomes in pneumonia patients even without evident heart disease. Kidney disease is killer number nine, and TMAO is strongly related to kidney function and predicts fatal outcomes there as well. Over a period of five years, more than half of chronic kidney disease patients who started out with average or higher TMAO levels were dead, whereas among those in the lowest third of levels, nearly 90% remained alive.
How can we lower the TMAO levels in our blood? Because TMAO originates from dietary sources, we could limit our intake of choline- and carnitine-rich foods. They’re so widespread in foods,” though we’re talking about meat, eggs, and dairy. “Therefore, restriction of foods rich in TMA-containing nutrients may not be practical.” Can we just get a vegan fecal transplant? “Vegan donors provided the investigators with a fresh morning fecal sample…”
If you remember, if you give a vegan a steak, despite all that carnitine, they make almost no TMAO compared to a meat-eater, presumably because the vegan hasn’t been fostering steak-eating bugs in their gut. See below and at 3:40 in my video Can Vegan Fecal Transplants Lower TMAO Levels?.
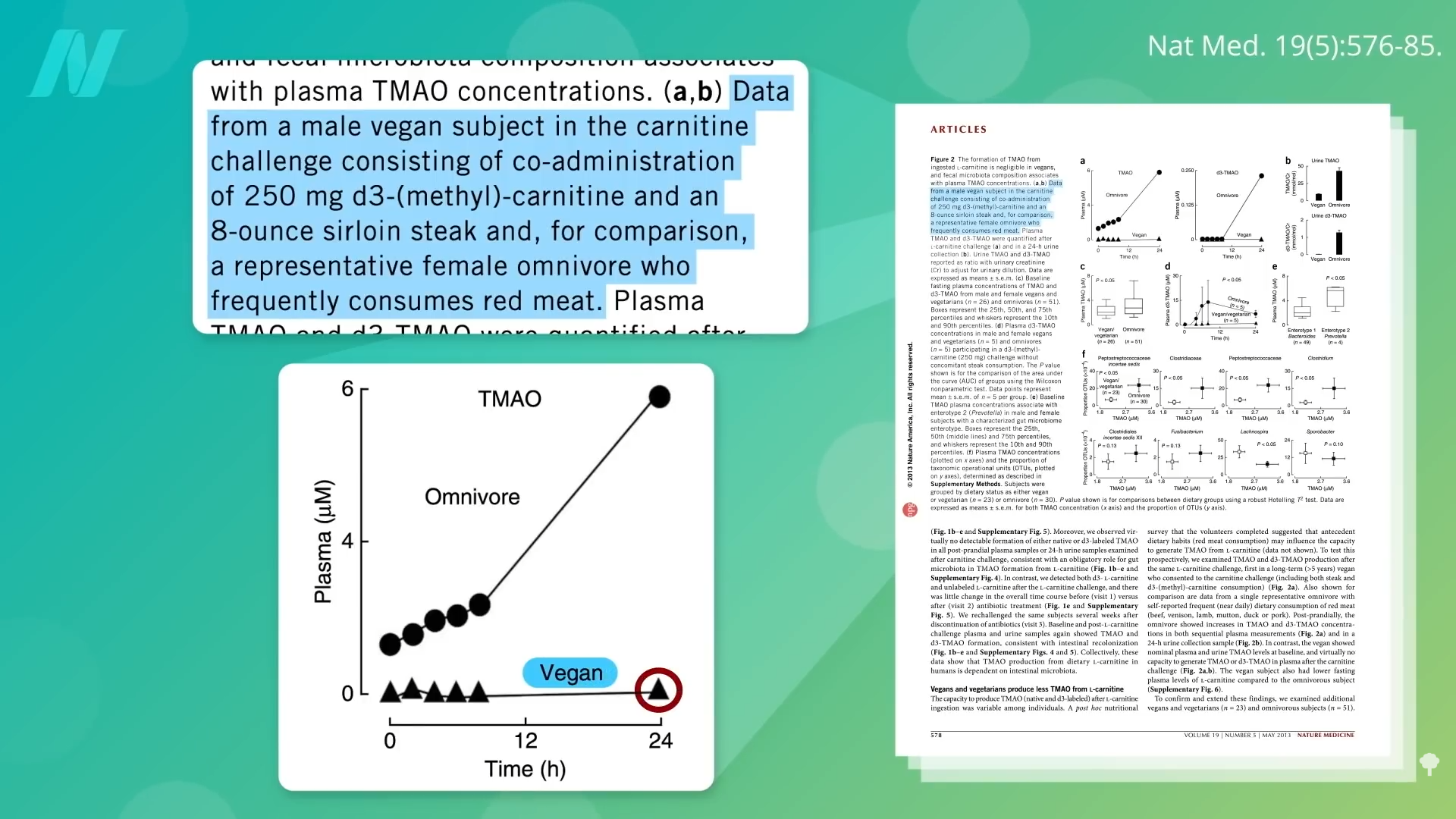
Remarkably, even if you give plant-based eaters the equivalent of a 20-ounce steak every day for two months, only about half start ramping up production of TMAO, showing just how far their gut flora has to change. The capacity of veggie feces to churn out TMAO is almost nonexistent. Instead of eating healthier, what about getting some vegan poop?
In a double-blind, randomized, controlled trial, research subjects either got vegan poop or their own poop back through a hose snaked down their nose, and it didn’t work.
First of all, the vegans recruited for the study started out making TMAO themselves, in contrast to the other study, where they didn’t make any at all. This may be because the earlier study required the vegans to have been vegan for at least a year, and this study didn’t. So, there wasn’t much of a change in TMAO running through their bodies two weeks after getting the vegan poop, but the vegan poop they got seemed to start out with some capacity to produce TMAO in the first place.
So, the failure to improve after the vegan fecal transplant “could be related to limited baseline microbiome differences and continuation of an omnivorous diet” after the vegan-donor transplant. What’s the point of trying to reset your microbiome if you’re just going to eat meat? Well, the researchers didn’t want to switch people to a plant-based diet since they knew that alone can change our microbiome, and they didn’t want to introduce any extra factors. The bottom line is that it seems there may not be any shortcuts. We may just have to eat a healthier diet.
Doctor’s Note
Want to become a donor? Find out How to Become a Fecal Transplant Super Donor.
For more on TMAO, check out related posts below.
See the microbiome topic page for even more.
from NutritionFacts.org https://nutritionfacts.org/blog/can-vegan-fecal-transplants-lower-tmao-levels/
via IFTTT
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Bernstein
via IFTTT
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Bradley
via IFTTT
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Johnson
via IFTTT
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Kovacs
via IFTTT
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Lewiecki
via IFTTT