from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Johnson
via IFTTT
Peter Kovacs, MD, PhD
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Kovacs
via IFTTT
E. Michael Lewiecki, MD
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Lewiecki
via IFTTT
JoAnn E. Manson, MD, DrPH
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Manson
via IFTTT
Susan J. Wysocki, RNC, NP, WHNP-BC
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/bios/ed-womenshealth#Wysocki
via IFTTT
Point-of-Care Medical Reference App For Doctors
Check drug interactions, access 450+ medical calculators, and ID pills at the point-of-care with Medscape’s official app. No hidden costs or subscription fees.
from Ob/Gyn & Women’s Health – Medscape https://www.medscape.com/public/medscapeapp?src=ban_strip_mscpmrk_app
via IFTTT
Is Aflatoxin a Concern?
Is “toxic mold syndrome” a real thing? What do we do about toxic mold contamination of food?
In recent years, mold has been blamed for all sorts of “vague and subjective” symptoms, but we have little scientific evidence that mold should be implicated. However, this “concept of toxic mold syndrome has permeated the public consciousness,” perpetuated by disreputable predatory practices of those making money testing homes for mold spores or testing people’s urine or blood. But all these tests are said to “further propagate misinformation and inflict unnecessary and often exorbitant costs on patients desperate for a clinical diagnosis, right or wrong, for their constellation of maladies…The continued belief in this myth is perpetuated by those charlatans who believe that measles vaccines cause autism, that homeopathy works, that fluoride in the water should be removed….”
Mold toxin contamination of food, however, has emerged as a legitimate issue of serious concern, and mycotoxins are perhaps even more important than other contaminants that might make their way into the food supply. Hundreds of different types have been identified, but only one has been classified as a known human carcinogen, and that’s aflatoxin. The ochratoxin I’ve previously discussed is a possible human carcinogen, but we know aflatoxin causes cancer in human beings. In fact, aflatoxins are amongst the most powerful known carcinogens.
It has been estimated that about a fifth of all liver cancer cases may be attributable to aflatoxins. “Since liver cancer is the third-leading cause of cancer deaths worldwide, and mortality rapidly follows diagnosis, the contribution of aflatoxins to this deadly cancer is significant.” And once aflatoxin makes it into the food, there is almost nothing we can do to remove it. Cooking, for example, doesn’t help. Indeed, as shown below and at 1:50 in my video Should We Be Concerned About Aflatoxin?, once it makes it into crops or into the meat, dairy, and eggs from animals consuming those crops, it’s too late. So, we have to prevent contamination in the first place, which is what we’ve been doing for decades in the United States. Because of government regulations, “companies in developed countries…are ‘always sampling’ for aflatoxin,” resulting in nearly $1 billion in losses every year. That may get even worse if climate change exacerbates aflatoxin contamination in the Midwest Corn Belt.

So, on a consumer level, it is more of a public health problem in the less industrialized world, such as in African countries, where conditions are ripe and farmers can’t afford to throw away $1 billion in contaminated crops. Aflatoxin remains a public health threat in Africa, Southeast Asia, and rural China, affecting more than half of humanity. This explains why the prevalence of liver cancer in those areas may be 30 times higher, yet it is not a major problem in the United States or Europe.
Only about 1% of Americans have detectable levels of aflatoxins in their bloodstream. Why not 0%? The U.S. Food and Drug Administration works to ensure that levels of exposure to these toxins are kept as low as practical, not as low as possible. In California, for instance, there has been an increase in “unacceptable aflatoxin levels” in pistachios, almonds, and figs. Unacceptable in Europe, that is, so it affects our ability to export, but not necessarily unacceptable for U.S. consumers, as we allow twice as much aflatoxin contamination.
Figs are unique since they’re “allowed to fully ripen and semidry on the tree.” This makes them “particularly susceptible to aflatoxin production.” It would be interesting to know about the fig-consuming habits of the 1% of Americans who were positive for the toxin. If figs were to blame, I’d encourage people to diversify their dried fruit consumption, but nuts are so good for us that we really want to keep them in our diets. The cardiovascular health benefits we get from nuts outweigh their carcinogenic effects; nut consumption prevents thousands of strokes and heart attacks for every one case of liver cancer. “Thus, the population health benefits provided by increased nut consumption clearly outweigh the risks associated with increased aflatoxin B1 exposure.”
So, we’re left with aflatoxin being mostly a problem in the developing world, and, because of that, it “remains a largely and rather shamefully ignored global health issue….” Where attention has been paid, it has been largely driven by the need to meet stringent import regulations on mycotoxin contamination in the richer nations of the world, rather than to protect the billions of people exposed on a daily basis.
Doctor’s Note
This is the last video in a four-part series on mold toxins. If you missed the others, check the related posts below.
from NutritionFacts.org https://nutritionfacts.org/blog/is-aflatoxin-a-concern/
via IFTTT
Are the Effects of Ochratoxin Concerning?
The overall cost-benefit ratio for mycotoxins depends on which food is contaminated.
Ochratoxin has been described as toxic to the immune system, developing fetus, kidneys, and nervous system, as well as being carcinogenic, but that is in animal studies. Ochratoxin “causes kidney toxicity in certain animal species, but there is little documented evidence of adverse effects in humans.” That’s why it’s only considered a possible human carcinogen.
Big Ag assures that current ochratoxin levels are safe, even among those who eat a lot of contaminated foods. The worst-case scenario may be young children eating a lot of oat-based cereals, but, even then, “their lifetime cancer risk is negligible.” Individuals arguing against regulatory standards suggest we can eat more than 42 cups of oatmeal a day and not worry about it. Where do they get these kinds of estimates?
They determine the so-called benchmark dose in animals—the dose of the toxin that gives a 10% increase in pathology—then, because one would want to err on the side of caution, divide that dose by 500 as a kind of safety fudge factor to develop the tolerable daily intake. For cancer risk, you can find the tumor dose—the dose that increases tumor incidence in lab animals by 5%—and extrapolate down to the ”negligible cancer risk intake,” effectively incorporating a 5,000-fold safety factor, as seen below and at 1:28 in my video Should We Be Concerned About the Effects of Ochratoxin?.
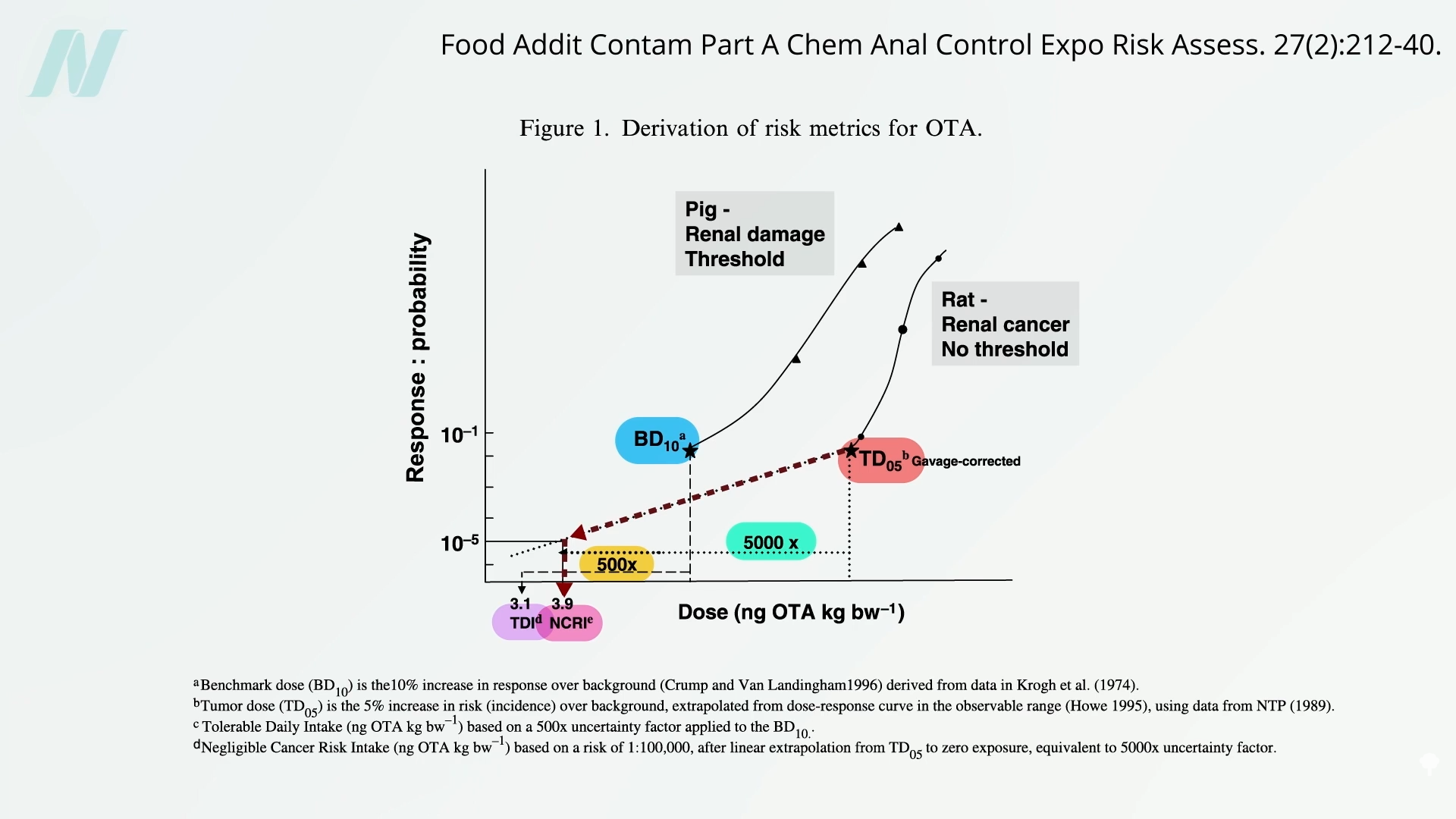
It seems kind of arbitrary, right? But what else are you going to do? You can’t just intentionally feed people the stuff and see what happens—but people eat it regularly. Can we just follow people and their diets over time and see if those who eat more whole grains, like oats, for example, are more likely to have cancer or live shorter lives?
What is the association between whole grain intake and all-cause, cardiovascular, and cancer mortality? Every additional ounce of whole grains eaten a day is associated with not only a lower risk for cancer mortality but also a lower risk of dying from all causes put together. Below and at 2:05 in my video are findings from all the big cancer studies. Every single one trended towards lower cancer risk.
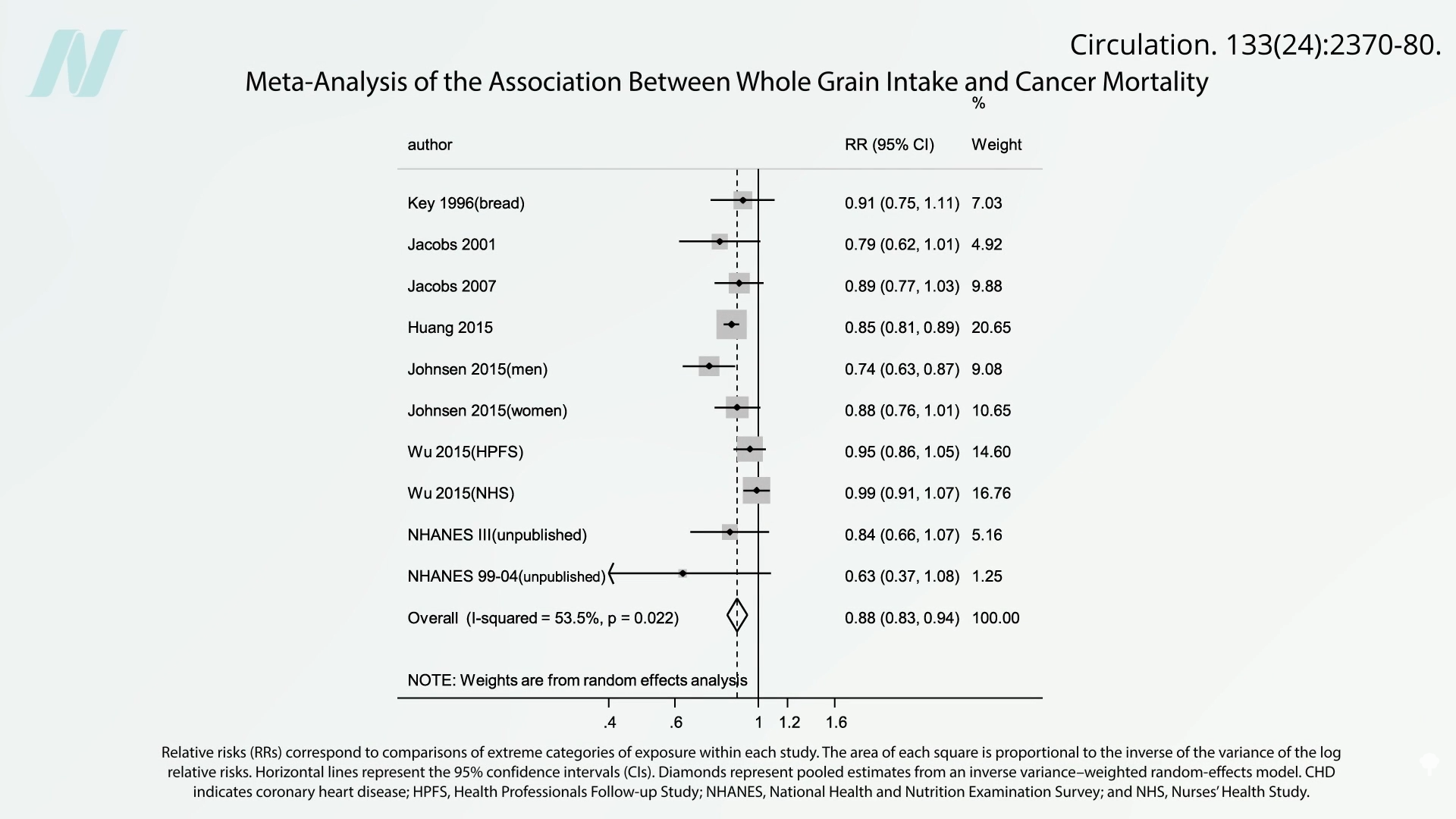
The bottom line is that you don’t find adverse effects confirmed in these population studies. This is not to say ochratoxin is necessarily harmless, but “any such risk does not outweigh the known benefits of wholegrain consumption.” In fact, healthy constituents of the whole grains themselves, like their antioxidants, may directly reduce the impacts of mycotoxins by protecting cells from damage. So, eating lots of fruits and vegetables may also help. Either way, “an overall healthy diet can play a significant role in mitigating the risk of contaminants in grain.”
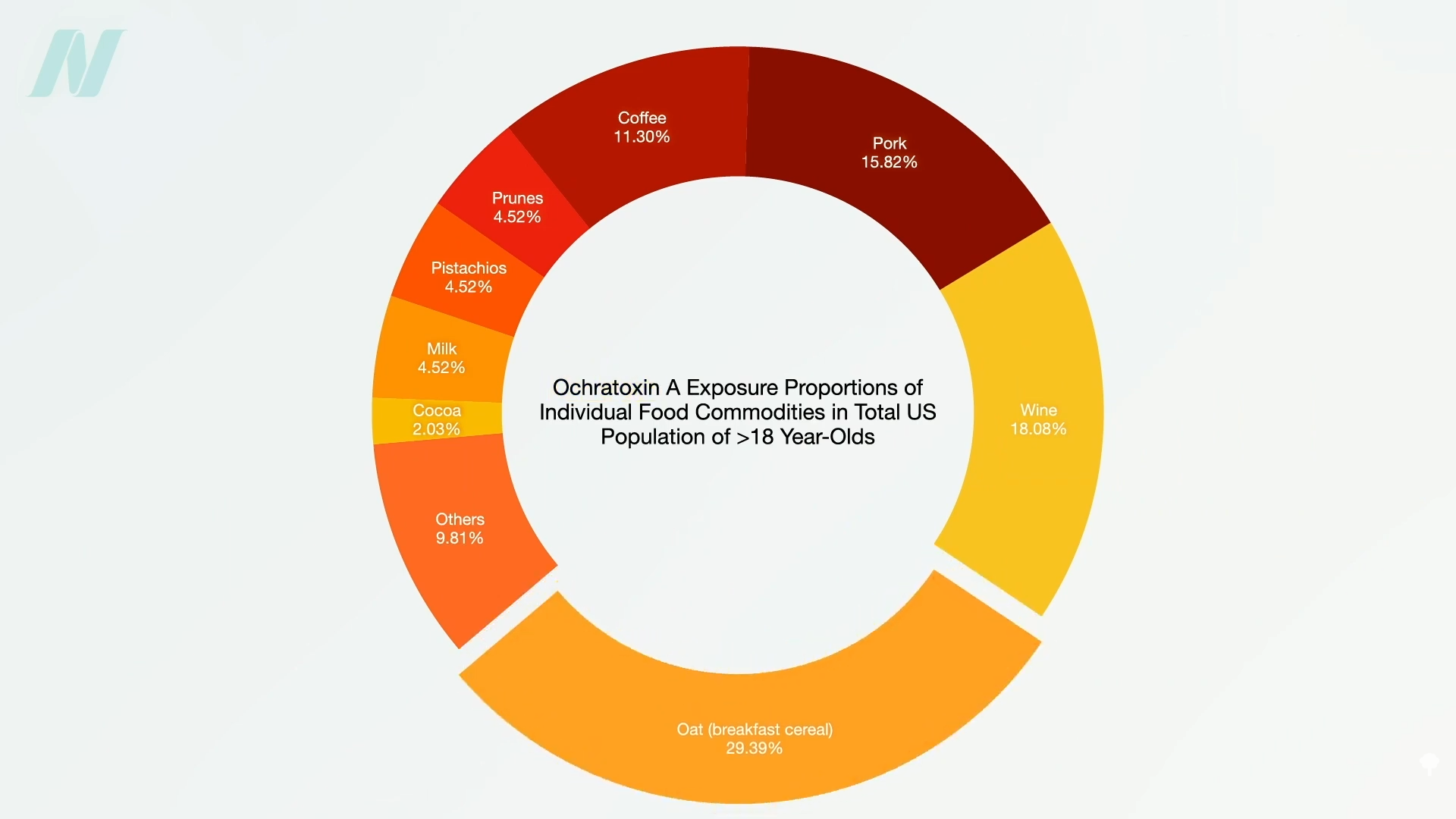
In summary, healthy foods like whole grains are good, but just not as good as they could be because of ochratoxin, whereas less healthful foods, like wine and pork, are worse because of the mycotoxin, as shown below and at 2:52 in my video. Ochratoxin was detected, for example, in 44% of tested pork.
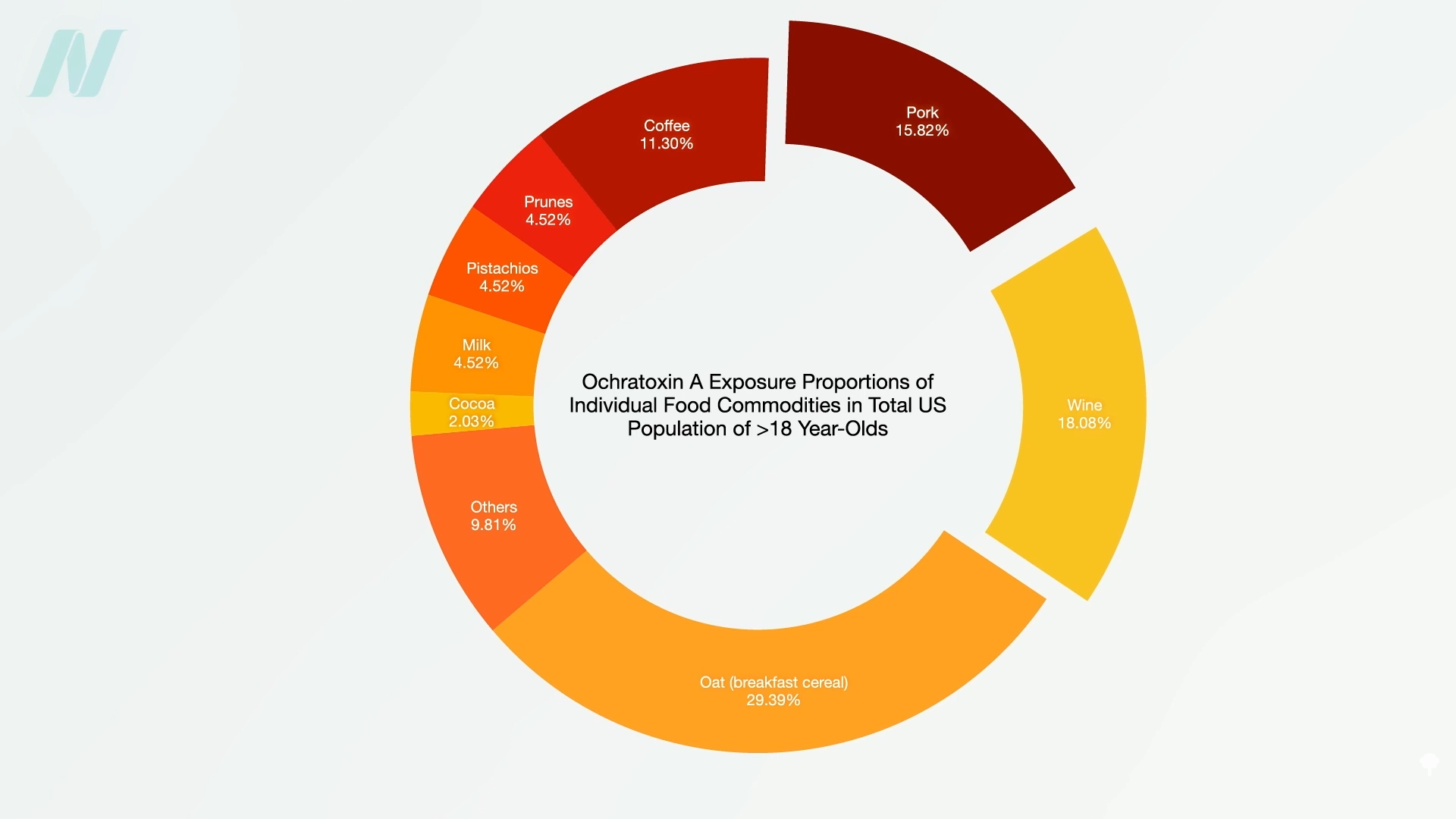
Doctor’s Note
This is the third video in a four-part series on mold toxins. If you missed the first two, see Ochratoxin in Breakfast Cereals and Friday Favorites: Ochratoxin and Breakfast Cereals, Herbs, Spices, and Wine.
Should We Be Concerned About Aflatoxin? is coming up next.
from NutritionFacts.org https://nutritionfacts.org/blog/are-the-effects-of-ochratoxin-concerning/
via IFTTT
Mold Toxins in Cereals, Herbs, Spices, and Wine
Most crops are contaminated with fungal mycotoxins, but some foods are worse than others.
Oats can be thought of as “uniquely nutritious.” One route by which they improve human health is by providing prebiotics that “increase the growth of beneficial gut microbiota.” There are all manner of oats, ranging from steel-cut oats to, even better, intact oat groats (their form before being cut), all the way down to highly processed cereals, like Honey Nut Cheerios.
“Rolling crushes the grain, which may disrupt cell walls and damage starch granules, making them more available for digestion.” This is bad because we want the starch to make it all the way down to our colon to feed our good gut bacteria. Grinding oats into oat flour to make breakfast cereals is even worse. When you compare blood sugar and insulin responses, you can see significantly lower spikes with the more intact steel-cut oats, as shown below and at 0:54 in my video Ochratoxin in Certain Herbs, Spices, and Wine.
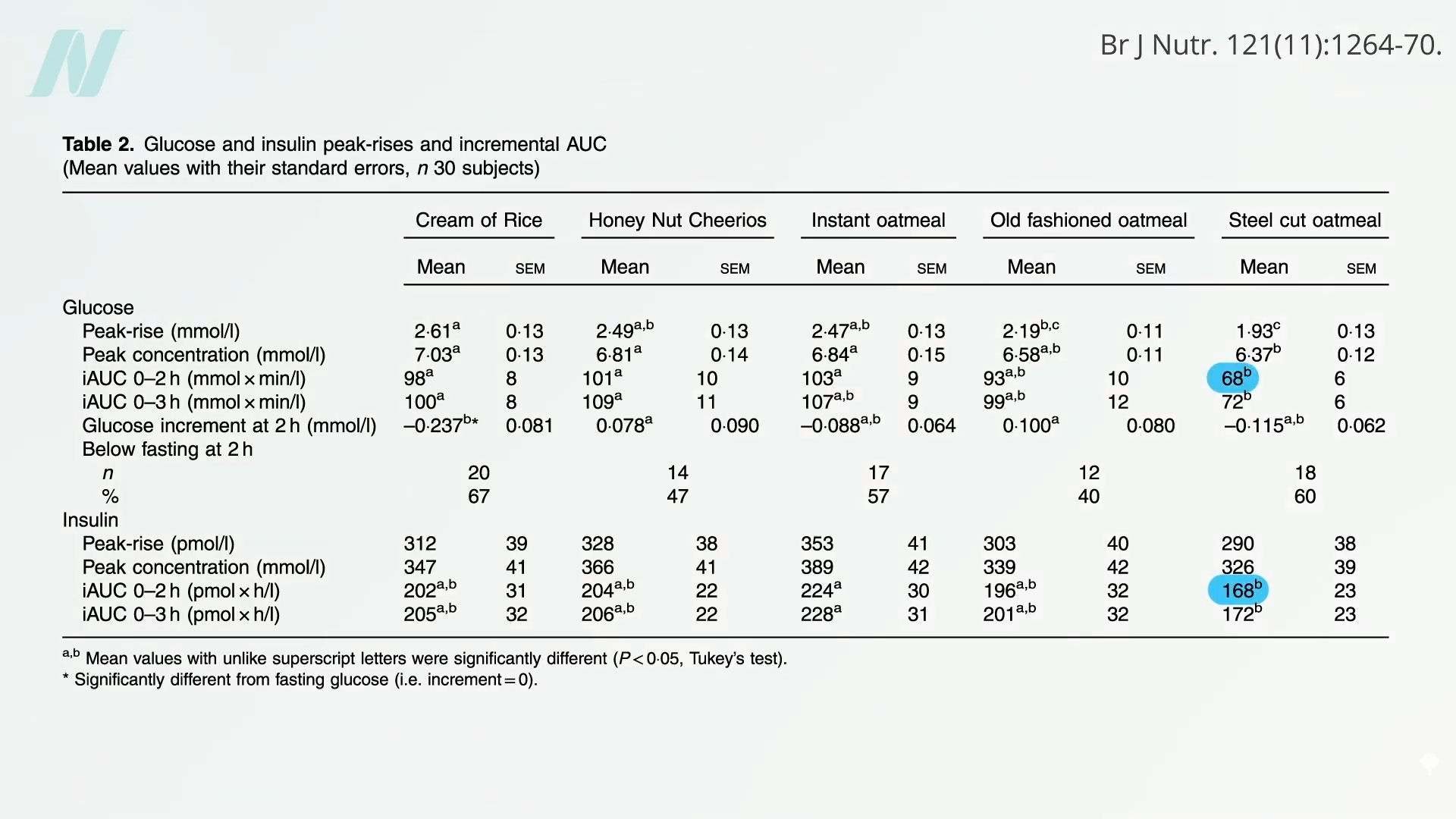
What about ochratoxin? As seen here and at 1:01 in my video, oats are the leading source of dietary exposure to this mold contaminant, but they aren’t the only source.
There is a global contamination of food crops with mycotoxins, with some experts estimating as much as 25% of the world’s crops being affected. That statistic is attributed to the Food and Agriculture Organization of the United Nations, but it turns out the stat is bogus. It isn’t 25%. Instead, it may be more like 60% to 80%. “The high occurrence is likely explained by a combination of the improved sensitivity of analytical [testing] methods and the impact of climate change.”
Spices have been found to have some of the highest concentrations of mycotoxins, but because they are ingested in such small quantities, they aren’t considered to be a significant source. We can certainly do our part to minimize our risk, though. For instance, we should keep spices dry after opening sealed containers or packages.
What about dried herbs? In “Mycotoxins in Plant-Based Dietary Supplements: Hidden Health Risk for Consumers,” researchers found that milk thistle–based supplements had the highest mycotoxin concentrations. It turns out that humid, wet weather is needed during milk thistle harvest, which is evidently why they get so moldy. “Considering the fact that milk thistle preparations are mainly used by people who suffer from liver disease,” such a high intake of compounds toxic to the liver may present some concern.
Wine sourced from the United States also appears to have particularly high levels. In fact, the single highest level found to date around the world is in a U.S. wine, but there’s contamination in wine in general. In fact, some suggest that’s why we see such consistent levels in people’s blood—perhaps because a lot of people are regular wine drinkers.
Ochratoxin is said to be a kidney toxin with immunosuppressive, birth defect–causing, and carcinogenic properties. So, what about ochratoxin decontamination in wine? That is, removing the toxin? Ideally, we’d try to prevent the contamination in the first place, but since this isn’t always practical, there is increased focus on finding effective methods of detoxification of mycotoxins already present in foods. This is where yeast enters as “a promising and friendly solution,” because the mycotoxins bind to the yeast cell wall. The thought is that we could strain out the yeast. Another approach is to eat something like nutritional yeast to prevent the absorption.
It works in chickens. Give yeast along with aflatoxin (another mycotoxin), and the severity of the resulting disease is diminished. However, using something like nutritional yeast as a binder “depends on stability of the yeast-mycotoxin complex through the passage of the gastrointestinal tract.” We know yeasts can remove ochratoxin in foods, but we didn’t have a clue if it would work in the gut until 2016. Yeast was found to bind up to 44% of the ochratoxin, but, in actuality, it was probably closer to only about a third, since some of the bindings weren’t stable. So, if you’re trying to stay under the maximum daily intake and you drink a single glass of wine, even if your bar snack is popcorn seasoned with nutritional yeast, you’d still probably exceed the tolerable intake. But what does that mean? How bad is this ochratoxin? We’ll find out next.
Doctor’s Note
This is the second video in a four-part series on mold toxins. The first one was Ochratoxin in Breakfast Cereals.
Stay tuned for Should We Be Concerned About the Effects of Ochratoxin? and Should We Be Concerned About Aflatoxin?. You can also check: Friday Favorites: Should We Be Concerned About Ochratoxin and Aflatoxin?.
from NutritionFacts.org https://nutritionfacts.org/blog/mold-toxins-in-cereals-herbs-spices-and-wine/
via IFTTT
The Effects of Fasting on Cancer
Ever since the days of Hippocrates, 2,400 years ago, fasting has been offered as a treatment for acute and chronic diseases, based on the observation that when people get sick they frequently lose their appetite.
Along with fever, decreased food consumption is one of the most common signs of infection. Often regarded as an undesirable manifestation of sickness, it’s actually an active, beneficial defense mechanism. As I discuss in my video Fasting for Cancer: What about Cachexia, chronic under-nutrition can impair our defenses, but data suggest that, in the short-term, immune function can be enhanced by lowering food intake.
Researchers have shown that the blood from starved mice was nearly eight times better at killing off the invading bacteria in a petri dish, dramatically boosting the capacity of their white blood cells to kill off the pathogens. What about people? And what about cancer?
Does Fasting Help Our Natural Killer Cells Fight Cancer Cells?
When study participants fasted for two weeks on an 80-calorie-a-day diet, not only did their white blood cells show the same kind of boost in bacteria-killing ability and antibody production, but their natural killer cell activity increased by an average of 24%. This is especially interesting because our natural killer cells don’t just help clear infections, but they also kill cancer cells. In fact, that’s how the researchers measured natural killer cell activity; they pitted them against K562 cells, which are human leukemia cells.
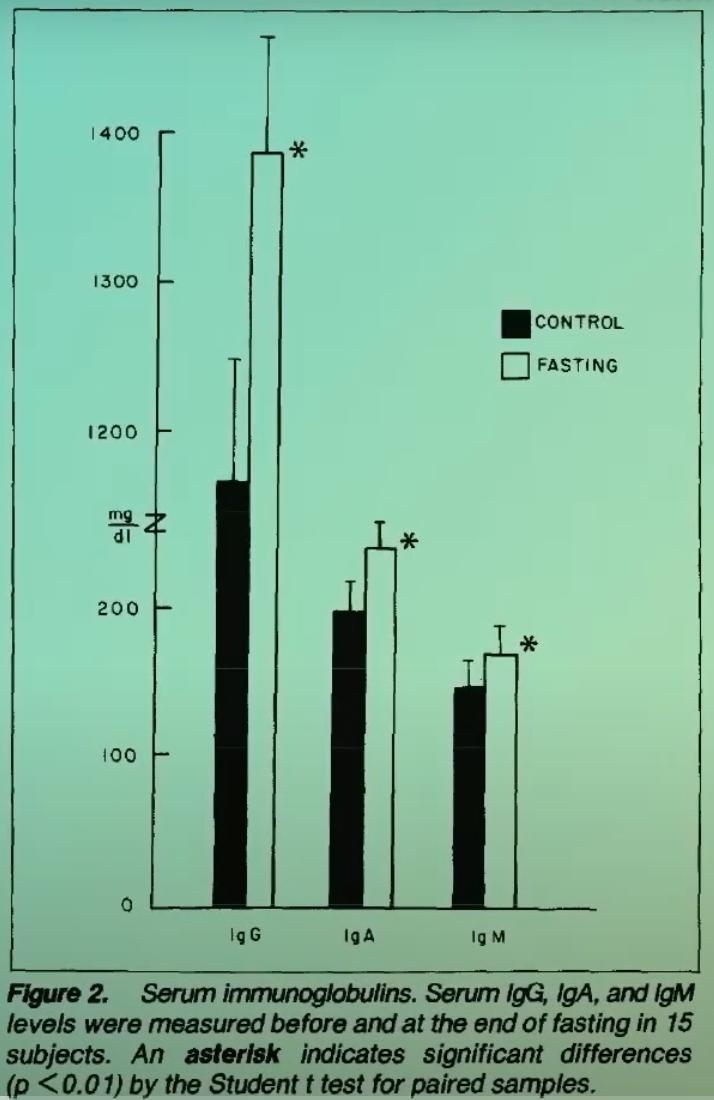
Fasting is said to improve anticancer immunosurveillance, or, more poetically, by “stimulating the appetite of the immune system for cancer.” So, why isn’t fasting used more to treat cancer? Because so much about cancer care revolves around keeping people’s weight up to try to counteract the cancer-wasting syndrome.
What Causes Cancer Cachexia?
Until recently, fasting therapy was not considered to be a treatment option in cancer, related to the fact that a common therapeutic goal in palliative cancer treatment is to avoid weight loss and counteract the wasting syndrome known as cachexia, which is the ultimate cause of death in many cancer cases.
Tumors are voracious, rapidly expanding and in need of a lot of energy and protein, so cancer metabolically reprograms the body to start breaking down to feed its tumors. It does this by triggering inflammation throughout the body. It’s not just that people lose their appetite. “The fundamental difference between the weight loss observed in CC [cancer cachexia] and that seen in simple starvation is the lack of reversibility with feeding alone.”
Therapeutic nutritional interventions to correct or reverse cachexia frequently fail. The best treatment for cancer cachexia, therefore, is to treat the cause and cure the cancer. In fact, maybe forcing extra nutrition on cancer patients could be playing right into the tumor’s hands. Like in pregnancy when the fetus gets first dibs on nutrients even at the mother’s expense, the tumor may be first in the feeding line. Maybe our loss of appetite when we get cancer is even a protective response.
Is Chemotherapy Enough?
As I discuss in my video Fasting Before and After Chemotherapy and Radiation, for the past 50 years, chemotherapy has been a major medical treatment for a wide range of cancers. Its main strategy has been largely based on targeting cancer cells, by means of DNA damage caused in part by the production of free radicals. Although these drugs were first believed to be very selective for tumor cells, we eventually learned that normal cells also experience severe chemotherapy-dependent damage, which can lead to dose-limiting side effects, including bone marrow and immune system suppression, fatigue, vomiting, diarrhea, and in some cases, even death.
If you do survive chemotherapy, the DNA damage to normal cells can even lead to new cancers down the road. There are cell-protecting drugs that have been tried to reduce the side effects so you can pump in higher chemo doses, but these drugs have not been shown to increase survival––in part because they may also be protecting the cancer cells. What about instead fasting for cellular protection during cancer treatment?
Fasting and Chemotherapy
Many may not recognize the role fasting can play in cancer prevention and treatment. Short-term fasting before and immediately after chemotherapy may minimize side effects, while, at the same time, it may actually make cancer cells more sensitive to treatment. That’s exciting!
During deprivation, healthy cells switch from growth to maintenance and repair, but tumor cells are unable to slow down their unbridled growth, due to growth-promoting mutations that led them to become cancer cells in the first place. This inability to adapt to starvation may represent an important Achilles’ heel for many types of cancer cells.
As a consequence of these differential responses of healthy cells versus cancer cells to short-term fasting, chemotherapy causes more DNA damage and cell suicide in tumor cells, while potentially leaving healthy cells unharmed. Thus, short-term fasting may protect healthy cells against the toxic assault of chemotherapy and cause tumor cells to be more sensitive––or at least that’s the theory.
Researchers found that, in rodents, fasting alone appears to work as well as chemotherapy. What’s more, unbridled tumor growth was also knocked down by radiation therapy—and even more so after the combination of radiation and alternate-day fasting. However, alternate-day fasting alone seemed to do as well as radiation. These data are exciting, but for mice with breast cancer. What about people?
Fasting Put to the Test Against Cancers
As I discuss in my video Fasting Before and After Chemotherapy Put to the Test, several patients diagnosed with a wide variety of cancers elected to undertake fasting prior to chemotherapy and share their experiences. They reported a reduction in fatigue, weakness, and gastrointestinal side effects while fasting and felt better across the board, with zero vomiting. The weight lost during the few days of fasting was quickly recovered by most of the patients and did not lead to any discernable harm. So, overall, fasting under care seems safe and potentially able to ameliorate side effects.
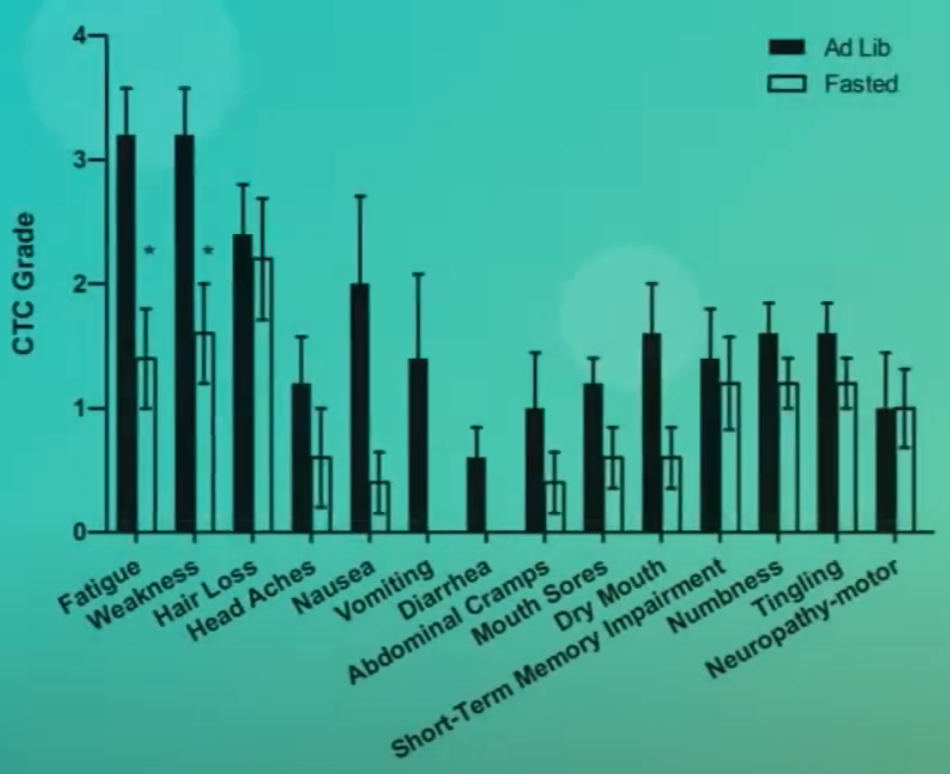
In a randomized clinical study, breast and ovarian cancer patients fasted from 36 hours before chemotherapy until 24 hours after, and fasting did appear to improve quality of life and fatigue. However, another study found no such beneficial effects. There did appear to perhaps be less bone marrow toxicity, given the higher counts of red blood cells and platelet-making cells. But no benefit when it came to saving white blood cells—the immune system cells—so that was a disappointment. Perhaps they didn’t fast long enough?
A systematic review of 22 studies found that, overall, fasting may not only reduce chemotherapy side effects (like organ damage, immune suppression, and chemotherapy-induced death), but it may also suppress tumor progression, including tumor growth and metastasis, resulting in improved survival. But, nearly all the studies were on mice and dogs. The studies on humans were limited to evaluating safety and side effects. The tumor-suppression effects of fasting––for example, its influence on tumor growth, metastasis and prognosis––sadly, were not evaluated.
Does Fasting Make Chemo More Effective?
As I discuss in my video Fasting-Mimicking Diet Before and After Chemotherapy, short-term food withdrawal during chemotherapy may begin to solve the long-standing problem with most cancer treatments: how to kill the tumor without killing the patient. Short-term fasting––for example, for 48 hours before chemo and 24 hours afterwards––may reduce side effects, so-called “chemotherapy-induced toxicity.” However, the potential tumor-suppressing effects of fasting have still not been thoroughly evaluated.
Some argue that reducing chemo’s side effects alone could improve efficacy, since patients could withstand higher doses. For example, the heart and kidney damage associated with the widely prescribed anti-cancer drugs limit their full therapeutic potential. It’s not clear, though, that maximizing the tolerated chemo dose would achieve longer survival or better quality of life. For now, I think we should just be satisfied with the fewer side effects for fewer side effects’ sake.
How Does Fasting Work?
Fasting can reduce the levels of insulin-like growth factor-1 (IGF-1), a cancer-promoting growth hormone. The reduced levels of IGF-1 mediate the differential protection of normal cells and cancer cells in response to fasting and improve chemo’s ability to kill cancer but spare normal cells.
So, reducing IGF-1 signaling may provide dual benefits by protecting normal tissues while reducing tumor progression. It may even help prevent the cancer in the first place. But fasting isn’t the only way to drop IGF-1 levels: A few days of fasting can cut levels in half, but that’s largely because protein intake is being cut. Protein is a key determinant of circulating IGF-1 levels in humans––suggesting that “reduced protein intake may become an important component of anticancer and antiaging dietary interventions,” particularly a reduction in animal protein.
Lowering Protein Intake to Lower IGF-1
If you compare those who eat strictly plant-based diets and get about the recommended daily intake of protein (0.8 grams per kg of body weight) to individuals who are just as slender but consume the higher amount of protein more typical to Americans, going on a calorie-restricted diet may lower IGF-1 a little, but eating a plant-based diet can lower it even more than going low calorie.
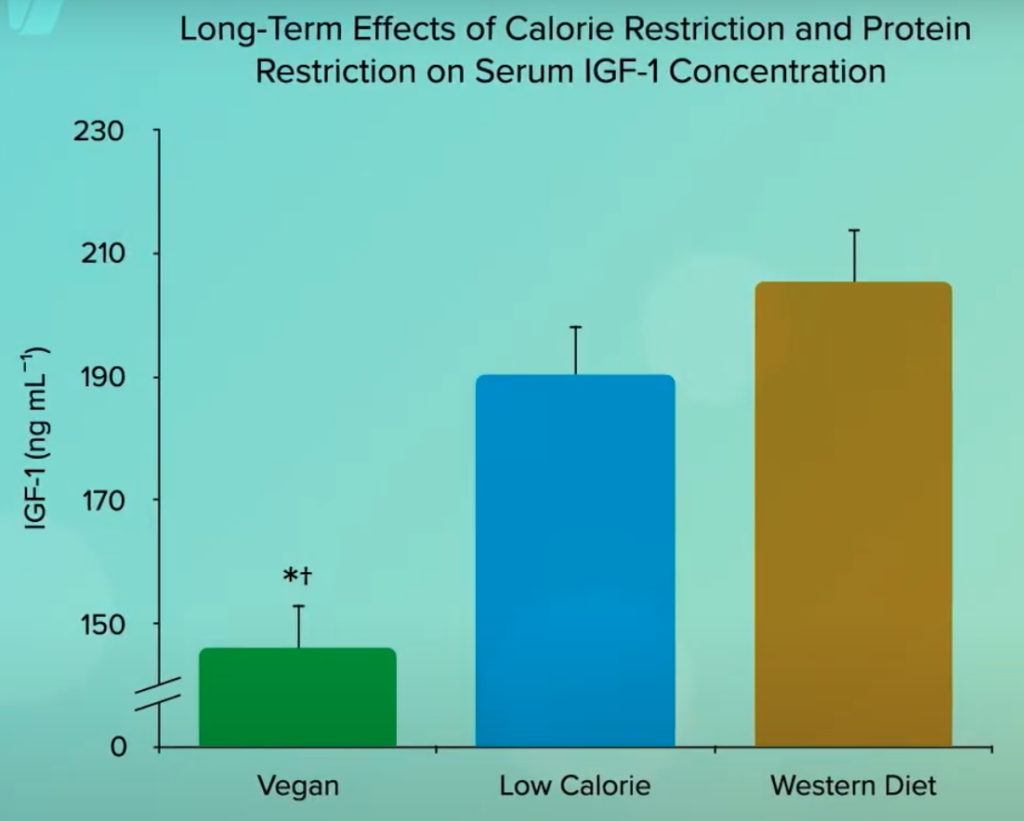
So, not only may a diet centered around whole plant foods down-regulate IGF-1 activity, potentially slowing the aging process, but it may be a way of turning anti-aging genes against cancer.
from NutritionFacts.org https://nutritionfacts.org/blog/the-effects-of-fasting-on-cancer/
via IFTTT